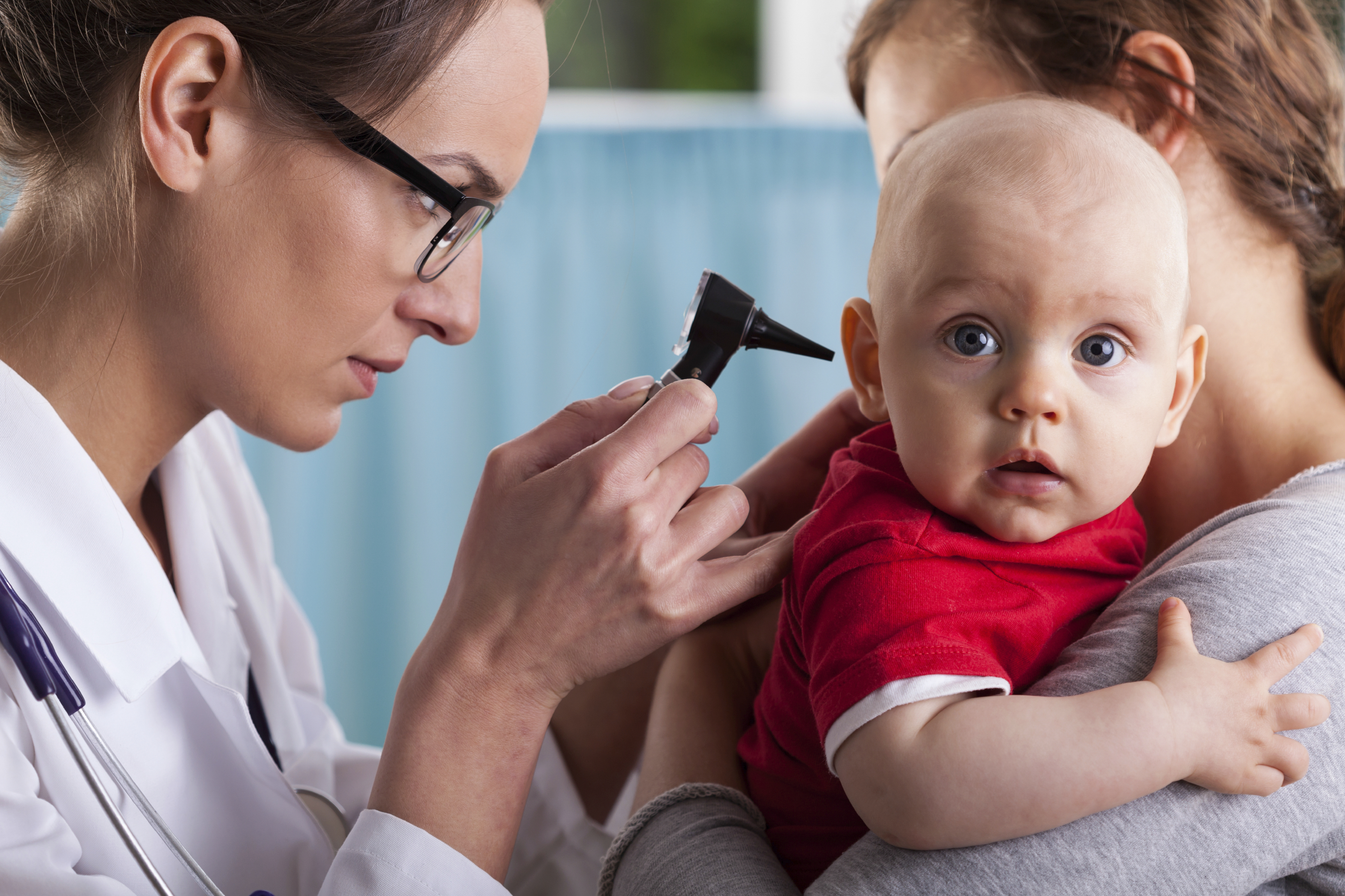
As a health writer, I know that ear infections are the #1 reason parents take their children to a doctor. As a parent, I know that ear infections are pure misery. I all too vividly recall the doctor's visit when my youngest was diagnosed with a double ear infection, her discomfort finally explained by a good look inside her ears.
There's been an interesting development in the world of ear infections, however. They're less common. A study published in the March issue of Pediatrics found that out of 367 study participants, 46 percent of infants developed an ear infection by the time they were 1. That might seem high until compared to studies in the 1980s and 1990s; the rate then was 60 percent. Infection rates were also lower for 3-month-olds (dropping from 18 to 6 percent) and for 6-month-olds (39 to 23 percent).
To learn more about these results and what they mean for parents, I talked with Dr. Wendy Sue L. Swanson, general pediatrician and executive director of digital health at Seattle Children's Hospital.
What are your thoughts on these results?
The big finding is that ear infection rates in infancy perhaps have gone down. Most people would attribute that to the availability of the pneumococcal vaccine [it was added to the recommended childhood vaccination schedule in 2000]. While this study looks at a lot of contributing factors that can lead to ear infections, I am surprised the rate is as high as it is, even if it has gone down. You flip a coin and ear infections are part of a child's infancy.

From a doctor’s perspective, what does this new research tell us?
There are many factors in the development of ear infections in infancy, primarily from infections caused by viruses or bacteria. But after six months, the way infants interact with the environment changed dramatically, as does their exposure to illness. For the first six months, they are held and protected. After six months, they can pick up an object, grasp it and put it in their month. The way they interact with the world has changed.
The researchers came away with two big changes. There is less smoking in the U.S., and they think decreased smoking affected the rate. Secondarily, now that babies receive the pneumococcal vaccine, they don't have as much streptococcus pneumoniae bacteria in their bodies,so the ear infections they found are often caused by other viruses or bacteria.
Is this study good news for parents?
What we can feel good about is that we think babies are protected from ear infections and the pain and discomfort caused by them in multiple ways. Infants receive robust protection from maternal antibodies from breastfeeding. If moms prolong breastfeeding, they will extend some of that protection. Secondarily, it's wonderful that infants are being protected from secondhand smoke. Lastly, we also believe vaccines have decreased the number of ear infections.
What's your advice for parents regarding ear infections in infants?
First and foremost, an ear infection in a child is a bunch of fluid, mucus and pus stuck behind the eardrum that can collect there after mucus develops anywhere in the sinus, throat and mouth areas. This happens after fluid backs up through the Eustachian tube, a connection between the back of the throat to the middle ear. The reason this matters is because ear infections are painful ... and can get in the way of hearing. Pediatricians want you to bring infants in if you suspect an ear infection at this critical time of hearing and language development.
Parents need to advocate for their infants so antibiotics are only used when necessary. Pediatricians need to get a good look at the infants' ear drums when diagnosing ear infections. If the doctor doesn’t get a good look or says "it looks red" or "there might be a little fluid" that doesn't qualify as diagnostic criteria for a middle ear infection that requires an antibiotic.
There are differences in timing of treatment for ear infections, too. We always recommend acetaminophen or pain medicines, but when and how we use antibiotics depends in part on diagnosis but also on age. In general, the American Academy of Pediatrics (AAP) recommends treating infants with ear infections with antibiotics from day one while waiting to treat toddlers with antibiotics until 48 to 72 hours have passed. That news hasn't changed since 2013. The 2013 AAP policy helps guide this care.
Learn more
Read up on ear infections in "An earful about ear infections." One highlight: Chronic ear infections might influence what your child eats.